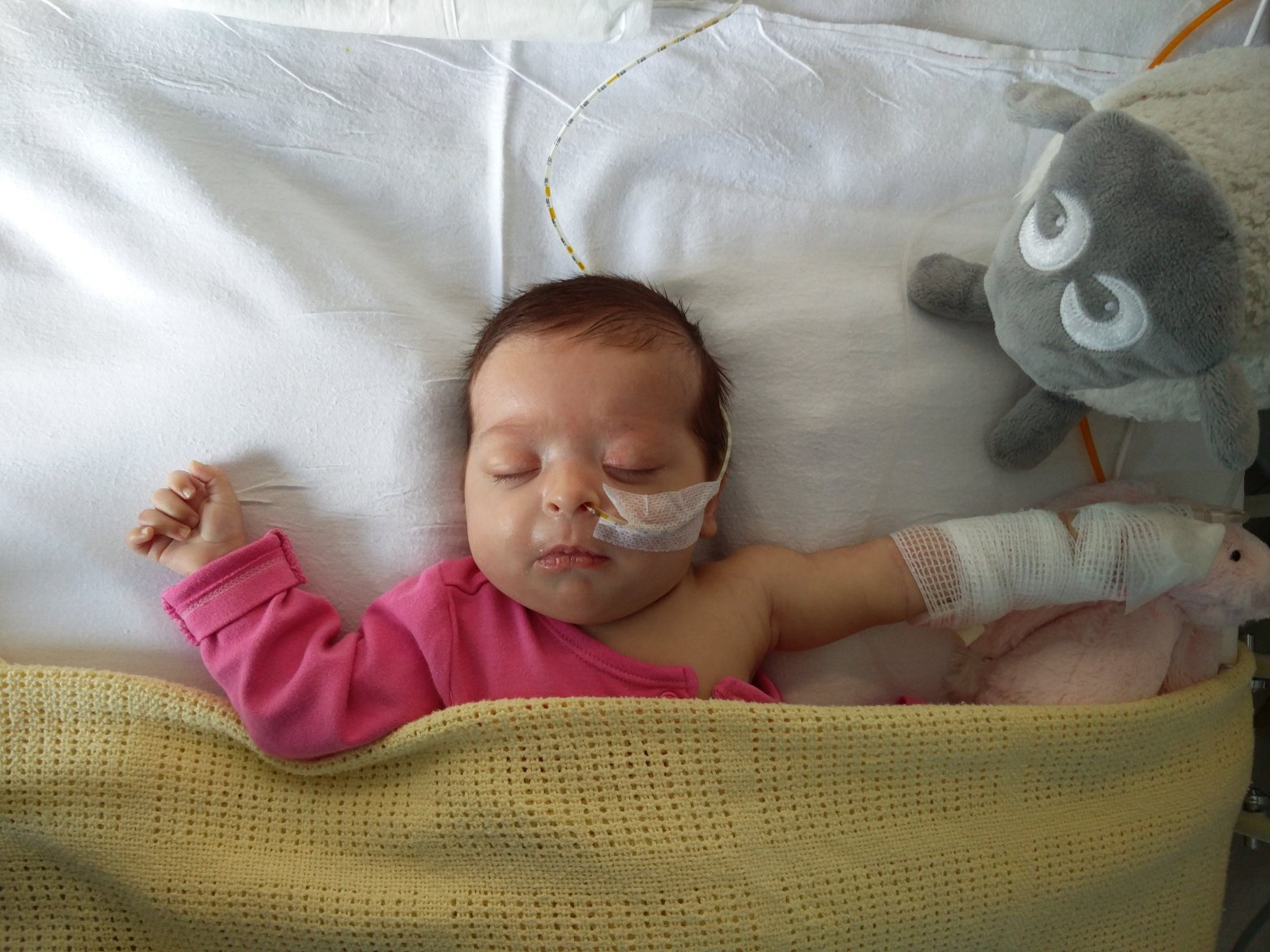
Thursday 8th March, 2018 – Clara had her bowel reconnected.
We’d known the date for weeks, it’s the first operation Clara’s had planned in advance. Contrary to what you might think, it was less worrying knowing it was coming. After all, this surgical procedure was a step in the right direction. A step towards home.
Clara was being given simple sugary hydration fluids the morning of her operation to keep her well as she needed to be nil by mouth before surgery. Brilliant, I thought, less weight on her Hickman Line. We planned to spend the morning cuddling in the window, I wanted to make the most of every minute I could get before surgery called.
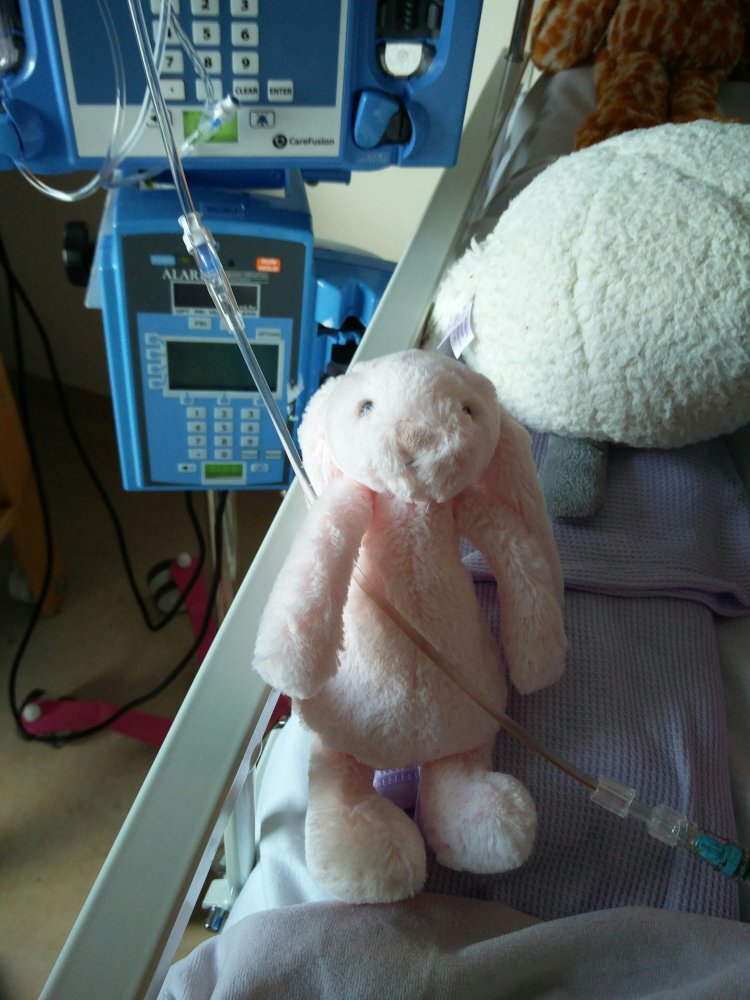
Unfortunately, the fluids were going through at a slower rate than her blood flow. So when I picked her up, gravity kicked in and her blood would flow from the main vein (that goes directly into her heart) down her hickman line instead, and into the fluid pipe. Sadly, this meant I couldn’t pick her up at all. So I hooked her pipe onto another hook on the fluid stand so it stayed above her heart level, and used Clara’s bunny Penny to keep the fluid pipe in place. It was upsetting I couldn’t cuddle Clara before such a huge operation, but I couldn’t risk her safety.
After walking Clara to the anesthetic room, next to theatre, it was time for Dean and I to keep ourselves distracted.
Five hours later, and two coffees with two slices of cake, and many shop windows browsed – we got the phone call . Clara’s surgery had finished and it had gone well. I’m not sure I’ll ever forget that phone call whilst strolling around Laura Ashley in Summertown. The relief flooded through us and it was time to race back to the car.
The surgical registrar, Natalie, had kindly agreed to call us before Clara was moved to recovery as that would give us a half an hour window to get back to the ward. 30 minutes later, I was able to go with the nurse to collect Clara. It’s indescribable how much it means to us when medical professionals remember their patients, and the families, are only human. It would have been easy for them to say they weren’t able to ring us, that we’d need to stick to procedures and the ward would be rung only when Clara was ready for collection. But they didn’t, they allowed us to get some breathing space out of the hospital, to stay distracted, and to be back in time. This small, but out of their way, gesture meant everything to us.
Clara came back to the ward in her cot. She has 1ml of morphine running continuously an hour, and paracetamol via IV. This morning that continues, she’s sleepy but wakes occasionally, opening her eyes slowly. Yesterday any jolting movement would cause her pain and she’d cry out, but today she’s able to move her arms and legs around without being in obvious discomfort.

Pictured below is the most alert she’s been, and it only lasted around a minute, but the small smile on her face tells me “things are going to be okay. I’ll feel back to my normal self soon mum”.
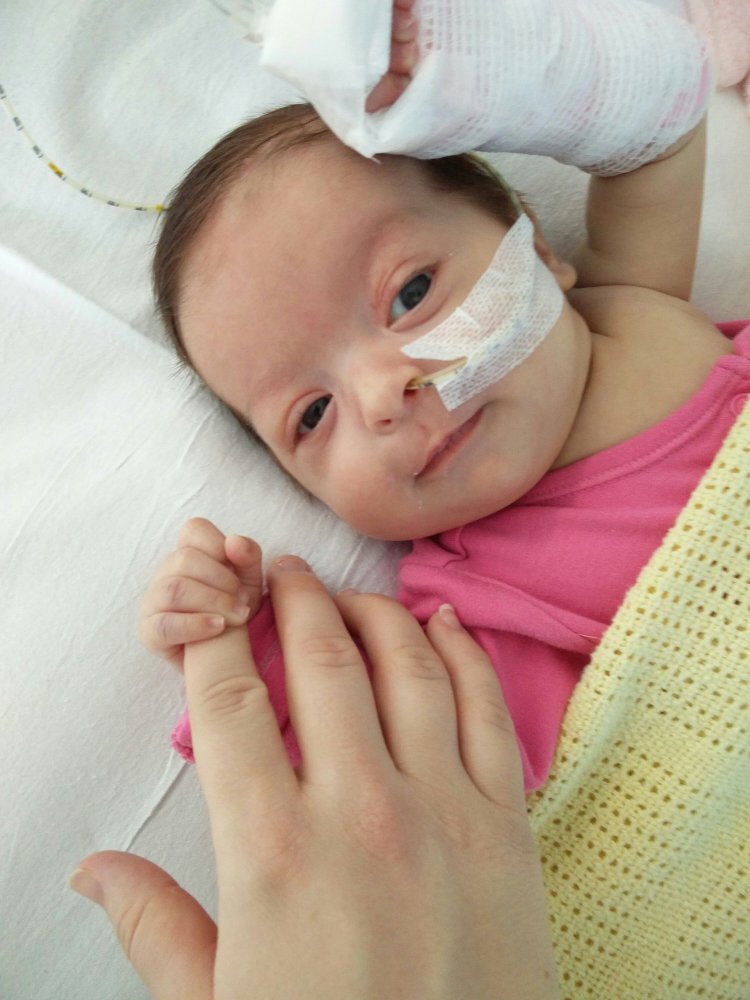
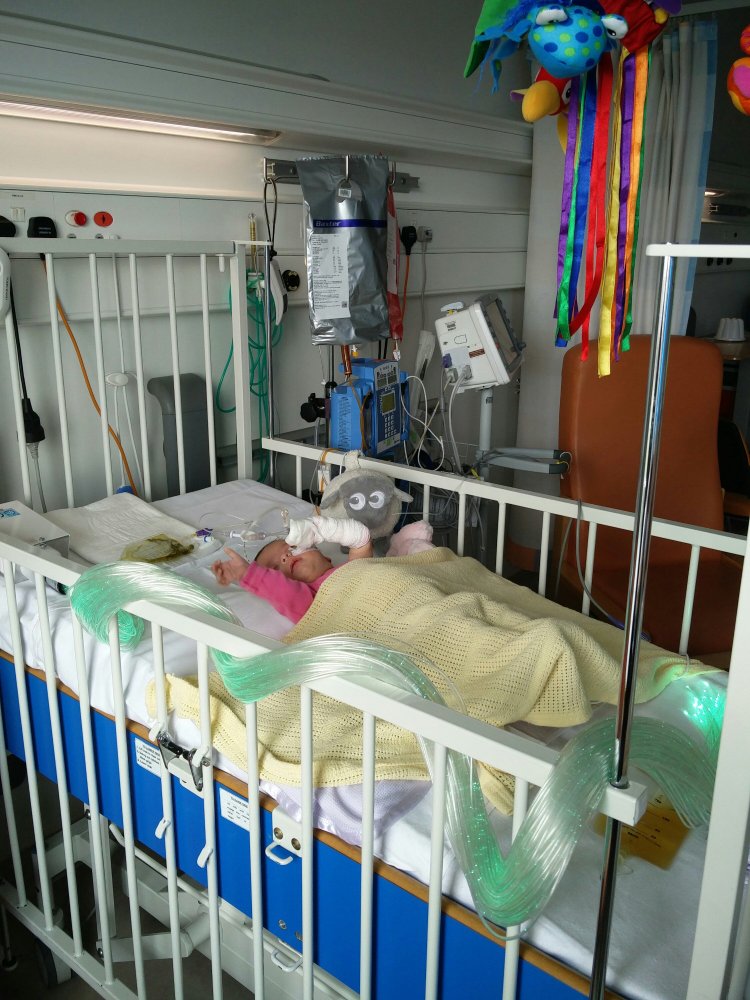
Clarissa, a play specialist, gave Clara these beautiful fibre optic lights that change colour every few seconds. When Clara does wake, she’ll have something to distract her from the pain.
So what happened in theatre?
The purpose of the operation was to connect Clara’s small intestine back together. Previously it had been split into three: the top part connected to her stomach; a little 5cm of small intestine that was still healthy that her surgeon saved last time but left closed up inside her; and the bottom 5cm of her small intestine attached to the colon.
In the process, her jejunostemy bag and pipe was removed as she no longer needed external drainage. The purpose of the bowel reconnection is to get her gut flowing the way it was designed to: out from her stomach all the way to her bottom.
Previously Clara had 33cm of healthy small intestine. Astonishingly, they discovered it had grown to 56.5cm! This is made up of 55cm connected to her stomach, and 1.5cm of the previous 5cm floating (each end had to be trimmed). Unfortunately we lost the bottom 5cm, which includes the valve to the colon. The valve helps slow down the flow, allowing more nutrition to be absorbed and less free flow straight to the bottom, but also helps minimise reflux. However, we can work without it now her bowel has grown so much, especially as it will continue to grow until she’s around 7 or 8 years old.
Clara will never have anywhere near the gut an ‘average’ person should have. She’ll suffer daily as a result, but her surgeon, Mr Lee, has given her the best fighting chance he can. Mr Lee and Natalie have given Clara her life back.
So what happens next?
Clara will be recovering for a while. She’ll stay on morphine, with a catheter in, for around a week. Hopefully not long after that she’ll start to feel a little happier and she’ll perk up. It’ll be a few weeks I imagine until she feels comfortably herself.
Longer term it means the focus shifts from the surgical team to the gastro intestinal specialists. Clara’s consultant will help us prepare for life looking after Clara with all of her special cares. This includes a few months of training on how to set up and take down Clara’s TPN fluids (we’ll be required to do this at home for a few years). I’m looking forward to this as it means it’s another way I can care for Clara, partly because the less people (and therefore less germs) that touch Clara’s hickman line the better, but also because as her mum I feel a duty to do all I can to help her.
It’s a long long road ahead, but I’ll take every step with Clara at her pace, holding her hand, and looking forward to those cheeky smiles!